Entradas
Mostrando las entradas de septiembre, 2014
| Lista de correo. Espere su aprobación. |
| Consultar este grupo |
Efficacy of a Educational Tool to Improve Handrubbing Technique in Healthcare Workers
- Obtener vínculo
- X
- Correo electrónico
- Otras apps
Addressing climate change in healthcare settings
- Obtener vínculo
- X
- Correo electrónico
- Otras apps
Future Projections for #ebola outbreak
- Obtener vínculo
- X
- Correo electrónico
- Otras apps
The durability of examination gloves used on intensive care units
- Obtener vínculo
- X
- Correo electrónico
- Otras apps
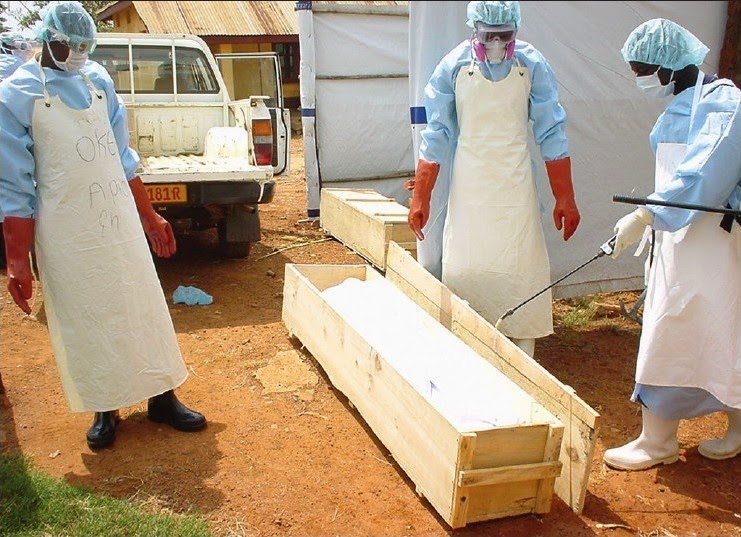
Reporte de casos de #ébola en trabajadores de la salud en África
- Obtener vínculo
- X
- Correo electrónico
- Otras apps
Fatal meningococcal disease in a laboratory worker - california, 2012
- Obtener vínculo
- X
- Correo electrónico
- Otras apps
UNICEF recruiting healthcare workers & other specialists
- Obtener vínculo
- X
- Correo electrónico
- Otras apps
WHO guidelines on hand hygiene in health care
- Obtener vínculo
- X
- Correo electrónico
- Otras apps
WHO Antimicrobial resistance: global report on surveillance 2014
- Obtener vínculo
- X
- Correo electrónico
- Otras apps
Reducing Needle Stick Injuries in Healthcare Occupations
- Obtener vínculo
- X
- Correo electrónico
- Otras apps
Infection Control During Filoviral Hemorrhagic Fever Outbreaks #Ebola
- Obtener vínculo
- X
- Correo electrónico
- Otras apps